A brief history of vaccines and an overview of their benefits.
Vaccines are the most cost-effective drugs available to date as they play an important role in the primary prevention of infectious diseases with a high percentage of efficacy, but they also prevent severe presentations of many illnesses when protection of contagion does not happen. The studies regarding their safety are also the most rigorous and highly powered among the field of medicine. Despite this, many concerns have been raised regarding the new anti-SARS-CoV-2 vaccines. In such setting it is important to remember what vaccines can do for the prevention and eradication of infectious diseases.
- Vaccines are the most cost-effective drugs on the history of medicine.
- They have served to erradicate diseases.
- They reduce the severity of diseases.
Vaccines; history; efficacy; primary prevention
Early history of vaccination
Smallpox was a viral disease that produced a persistent fever of 38-40°C, attack to the general state, headache, vomiting and, importantly, bulging skin eruptions that tended to fill themselves with liquid to form blisters that depressed in the middle and fell off to leave the dermis, and sometimes the sub-dermis, exposed in multiple sites of the body. Thus, these pustules posed an increased risk for infected patients to develop bacterial skin coinfections, which worsened the prognosis. The illness also made many survivors blind for life. In this way Smallpox had a lethality of 20-60%, and killed 70% of pregnant women that became infected, and the survivors were always scarred for life (Fig. 1) (1, 2).
There are no records of the date of origin of this disease, but it is believed that it dated back to the Egyptian Empire around the 3rd century BCE, and by the 16th century it had spread worldwide. In this way, it is impossible to make an accurate assessment of how many people was killed by smallpox, but it is estimated that this disease killed 400,000 Europeans each year in the 18th century (3), and killed 300 million people in the 20th century alone. Thus, it is considered as the disease that has killed more people in the history of mankind (4). The dread it caused has been an important subject of public knowledge and popular culture since the origins of civilization, but it all came to an end with the practice of vaccination.
Vaccination originated from an ancient Asian practice called variolation, which consisted on making incisions on the shoulders or arms of the patients and inoculating them with materials from drying pustules of smallpox infected patients. Variolation was the best prophylactic measure against such a dreadful disease that was available in the 18th century, as it reduced the lethality of the disease to 1 in 50 in its beginnings, and to 1 in 500 when the technique was further refined (5), but it could not reduce its incidence. Moreover, this practice was deemed as unsafe as it produced strong fevers, and sometimes the patients that were intended to be protected became infected (if the materials from the pustules were not dried, and thus inactivated, enough), or developed further infections that led to amputations or septic shocks (as the pustules tended to contain live bacteria or bacterial spores).
Edward Jenner (Fig. 2), the father of immunology, virology and vaccinology was one of those patients whom recalled with horror the strong fevers and fears that came in the post-variolation isolation periods, as he was variolated as a boy. Despite this, he still performed variolation with his patients as he believed in the preventive power of such practice, but he was in constant fear for his patients’ health after such immunizations. On the other hand, he was aware of the country lore that milkmaids who became infected with cowpox from their cows were unable to catch smallpox later. He then, in 1976, extracted the liquid from the pustules of a local milkmaid, named Sarah Nelmes, who had cowpox at that time, and inoculated such fluids to James Phipps, his gardener’s son. Afterwards he exposed the boy to smallpox, only to find him immune to such disease (6). Jenner published his results two years later (7), to induce controversy within the scientific community, but also a general acceptance by the general public, as his vaccine (named after the Latin vacca, or cow), provided a more effective and safe approach to smallpox prevention than variolation.
Since prior to vaccination nearly everyone contracted the disease at some point in their lives, being that smallpox possessed a basic reproductive number estimated between 3 and 6 (meaning that each infected person would transmit the disease to an average of 3 to 6 other patients), vaccination came to grate success to the general public´s opinion, and thus it started to being spread throughout the world (8). Jenner himself devoted his life to apply his vaccine freely to anyone who requested it, while other physicians did the same outside of England.
After the introduction of smallpox to the Americas in 1520, Jenner’s vaccine was a necessity in the newly discovered continent, until Alonso Núñez de Haro in 1863 donated part of his properties to constitute the first vaccination center in the Americas. The vaccine had to be carried from Europe by a serial vaccination of the crew members of a ship, in order for it to arrive viable into the new continent (1). Later in 1966, the World Health Organization (WHO) embarked on a program to completely eradicate smallpox from the entire world, following the idea that John Haygarth and Jenner himself originally proposed at their time. That vaccination campaign was the biggest in history and continued until in 1979 the world saw its first day without a single case of smallpox. A condition that remained a year later, causing the WHO´s declaration of eradication to come, and has fortunately enough maintained until today.
In this instance, the WHO considers that the smallpox vaccine has saved more than 10 billion lives since its invention, and $1,000 million of USD every year, regarding Jenner as the man who has saved more lives in the history of mankind (9), and vaccines as the most cost-effective and beneficial drugs of all time.
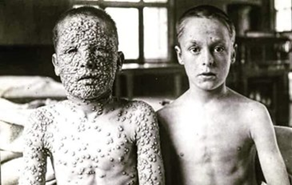
Fig. 1. Vaccinated and unvaccinated twins. The twin on the right recieved proper vaccination at a younger age, while the twin at the left was not vaccinated and therefore became ill with smallpox. The picture shows the typical scarring that smallpox produced in its survivors.
.png)
Fig. 2 Edward Jenner. Oil painting from an unknown author. Dr. Jenner´s house. Museum and garden. Berkeley, England.
The golden age of vaccines
After Jenner’s work no other vaccines were developed due to the lack of knowledge in immunology and microbiology, nonetheless, in 1878 Louis Pasteur discovered that the passage of one microbe through several in vitro cultures caused the attenuation of the microbes, a knowledge that paved the way for the development of other vaccines. Thus, in 1881 Pasteur was able to develop an anti-anthrax vaccine, and four years later he was able to develop the anti-rabic vaccine. Several new vaccines were developed in the following decade by attenuating the microorganisms that caused the diseases, either by the Pasteur’s technique or by physical and chemical means. The next leap on vaccine technology came from Émile Roux and Alexandre Yersin, who recognized the importance of the bacterial toxins in diphtheria and tetanus, isolated the toxins and chemically inactivated them, thus leading the development of sub-unitary vaccines, a technology where subunits of the disease-causing microorganisms is used to immunize the patients (10).
It was later discovered that immunization, and therefore vaccines, work by mimicking an infection in the body of a patient, through the administration of i) a live, but attenuated microorganism (like Pasteur’s vaccines), or alternatively with microorganisms that are not infectious to humans but possess an analogical structure to the ones that do (like Jenner’s vaccine), and finally ii) with subunits from the human pathogens. These biologic preparations are thus unable to cause disease, but nonetheless produce an immune response where the lymphocytes that possess the specific receptors to recognize the antigens in the vaccine proliferate copiously. Many of these lymphocytes will destroy the components of the vaccine and die after ≈21 days, but about 30% of them will prevail as memory cells. In the event of a further exposition to the same antigens that formulated the vaccine (and therefore the pathogen that produces them), these memory cells are able to quickly proliferate and attack the microbe before it has time to colonize and affect the host (11).
The benefits of vaccination
No other human disease has ever been eradicated; nonetheless it is believed that poliomyelitis would be the next illness to be eradicated, as it is now endemic to only Pakistan, Nigeria and Afghanistan, where continued war and extreme poverty have obstructed the humanitarian vaccination efforts.
Vaccines can effectively protect 39 to 98% of vaccinated people (12), of 27 vaccine-preventable diseases (13), thus lowering the rate of transmission even for non-vaccinated people, or patients whom received a vaccine but the drug did not protected them, as vaccines can produce herd immunity when ≈70% of population has been vaccinated (14). Even when a vaccine does not prevent disease, it can lower the severity of disease presentation (15). Thus, there has been a 99% decrease in incidence for the nine diseases for which vaccines have been applied universally, accompanied by a similar decline in mortality and disease sequelae (16), saving at least 6 million lives annually (17). This has impacted on the elimination of several diseases from many countries where extensive vaccination is applied, and led to the complete eradication of smallpox and of two of three types of poliomyelitis (18).
Global economy also benefits from vaccination as such strategy was estimated in 2003 to cause savings in the order of tens of billions of dollars each year (19) (Fig. 3). Moreover, the reduction of the incidence of diseases by vaccination programs impacts directly in healthcare and treatment costs (20), decreasing both medical interventions and population’s time off work (21). A good example of the economic benefit of vaccines is the smallpox eradication, allowing millions of dollars saved annually, as mentioned previously. Additionally, vaccination effects in morbidity and mortality lead to more children surviving to adulthood, representing an increase in economically active population (21, 22). Moreover, vaccines in epidemics and pandemics can mitigate economic outcomes, leading to an effective control measure of emerging pathogens and their consequences (22). In such setting, it is expected that anti-SARS-CoV-2 vaccines will help to stabilize the current public health and economic crisis and lay the basis for a future response to infectious diseases.
Fig. 3: Vaccine benefits. Vaccines reduce the probability of patients to become infected; moreover, when enough patients have been vaccinated the probability of people that have not received the vaccine to become ill lowers as well, because the number of potential transmitters becomes reduced. As a consequence, disease incidence and prevalence becomes reduced, saving lives and money.
Conclusions
Since ancient time, infectious diseases have represented an important public health problem and are responsible of high morbidity and mortality rates. Vaccines development passed through several years of experimentation, and with science progresses, their diversity, effectiveness and security were improved. Thus, vaccination constitutes a highly cost-effective measure to prevent and control infectious diseases. Even though only few pathogens have been eradicated, vaccines have led to a considerable decrease of the incidence and severity of these illnesses, which finally represent millions of lives saved.
References
1. Navarrete Peón A. 2018. Educación para la salud: Editorial MX. 228 pp.
2. Behbehani AM. 1983. The smallpox story: life and death of an old disease. Microbiol Rev 47: 455-509
3. Riedel S. 2005. Edward Jenner and the history of smallpox and vaccination. Proc (Bayl Univ Med Cent) 18: 21-5
4. Centers of DC. 2016. History of Smallpox. Online: Centers of Disease Control
5. Boylston AW. 2002. Clinical investigation of smallpox in 1767. N Engl J Med 346: 1326-8
6. Stewart AJ, Devlin PM. 2006. The history of the smallpox vaccine. J Infect 52: 329-34
7. Jenner E. 1749. An inquiry into the causes and effects of the variolae vaccinae: a disease discovered in some of the western counties of England, particularly Gloucestershire, and known by the name of the cow pox: Cooley, Samuel. 116 pp.
8. Lofquist JM, Weimert NA, Hayney MS. 2003. Smallpox: a review of clinical disease and vaccination. Am J Health Syst Pharm 60: 749-56; quiz 57-8
9. Kickbusch I. 1995. World Health Organisation: change and progress. BMJ 310: 1518-20
10. D'Amelio E, Salemi S, D'Amelio R. 2016. Anti-Infectious Human Vaccination in Historical Perspective. Int Rev Immunol 35: 260-90
11. Pulendran B, Ahmed R. 2011. Immunological mechanisms of vaccination. Nat Immunol 12: 509-17
12. Amanna IJ, Slifka MK. 2020. Successful Vaccines. Curr Top Microbiol Immunol 428: 1-30
13. Principi N, Esposito S. 2019. Vaccine-preventable diseases, vaccines and Guillain-Barre' syndrome. Vaccine 37: 5544-50
14. Andre FE, Booy R, Bock HL, Clemens J, Datta SK, John TJ, Lee BW, Lolekha S, Peltola H, Ruff TA, Santosham M, Schmitt HJ. 2008. Vaccination greatly reduces disease, disability, death and inequity worldwide. Bull World Health Organ 86: 140-6
15. van Dam ASG, Woudenberg T, de Melker HE, Wallinga J, Hahne SJM. 2020. Effect of vaccination on severity and infectiousness of measles during an outbreak in the Netherlands, 2013-2014. Epidemiol Infect 148: e81
16. Centers for Disease C, Prevention. 1999. Impact of vaccines universally recommended for children--United States, 1990-1998. MMWR Morb Mortal Wkly Rep 48: 243-8
17. Ehreth J. 2003. The global value of vaccination. Vaccine 21: 596-600
18. Fine PE, Griffiths UK. 2007. Global poliomyelitis eradication: status and implications. Lancet 369: 1321-2
19. Ehreth J. 2003. The value of vaccination: a global perspective. Vaccine 21: 4105-17
20. Deogaonkar R, Hutubessy R, van der Putten I, Evers S, Jit M. 2012. Systematic review of studies evaluating the broader economic impact of vaccination in low and middle income countries. BMC Public Health 12: 878
21. Rodrigues CMC, Plotkin SA. 2020. Impact of Vaccines; Health, Economic and Social Perspectives. Frontiers in microbiology 11: 1526-
22. Bloom D, Canning D, Weston M. 2005. The Value of Vaccination. World Economics 6: 15-39
Widget de imagen
Widget de imagen
Widget de imagen
 0
0
 0
0